The state of Oklahoma's behavioral health workforce
The federal government designates all 77 Oklahoma counties as mental health professional shortage areas. With few exceptions, Oklahoma's supply of behavioral health care providers is not sufficient to meet the demands of the state's population.
To grow the state’s behavioral health workforce, Oklahoma must attract prospective students to behavioral health degree programs that are high-quality, accessible, and affordable. Perhaps even more critical is ensuring the availability of “capstone” experiences — such as internships and residencies — that prepare individuals to become licensed professionals in Oklahoma.
Healthy Minds' latest research of the state of Oklahoma's behavioral health workforce includes two reports that examine these challenges:
- Greatest needs of Oklahoma's behavioral health workforce
This report explores Oklahoma’s behavioral health workforce shortages in greater detail, highlights improvements made in the state since 2020, and offers suggestions to enhance Oklahoma’s data collection practices. - Strengthening Oklahoma’s pipeline of behavioral health professionals
This report catalogues the educational opportunities available to professionals and paraprofessionals, identifies opportunities for improving employee recruitment and retention, and explores training and development opportunities that expand employees’ skills.
Policymakers have realistic options for addressing the state's most pressing behavioral health workforce challenges. With roughly $30 million in targeted funding and policy initiatives, Oklahoma can significantly strengthen workforce pipelines to meet the state’s growing need for behavioral health professionals. This can be accomplished through:
- Incentivizing students into expedient training pathways
- Expanding training that fuels in-state retention of critically needed clinicians
- Enhancing educational programs tailored to treatment system needs
- Providing upskilling opportunities for paraprofessionals
- Improving collection and use of behavioral health workforce data
Read a one-page summary of our key findings and recommendations for policymakers
Greatest needs of Oklahoma's behavioral health workforce
Read the full report
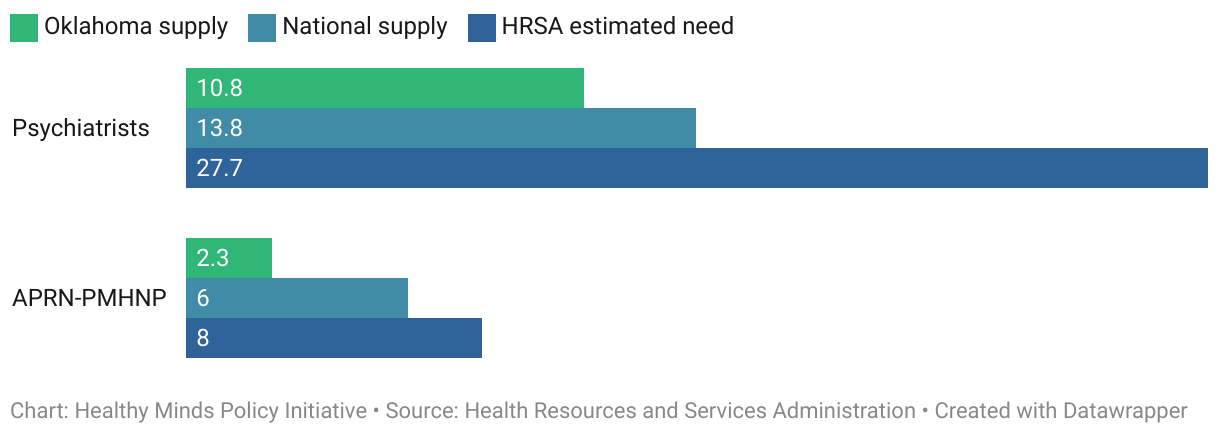
The greatest need for behavioral health providers in Oklahoma is for psychiatric prescribers. The federal Health Resources & Services Administration (HRSA) estimates that communities need 27.7 psychiatrists and eight psychiatric mental health nurse practitioners (APRN-PMHNPs) per 100,000 residents. Combined, states need an estimated 35.7 psychiatric providers per 100,000 residents, whereas Oklahoma’s combined supply is 13.1 per 100,000 residents. To fill this gap, the state must add psychiatry residency positions that attract and retain psychiatrists in the state.
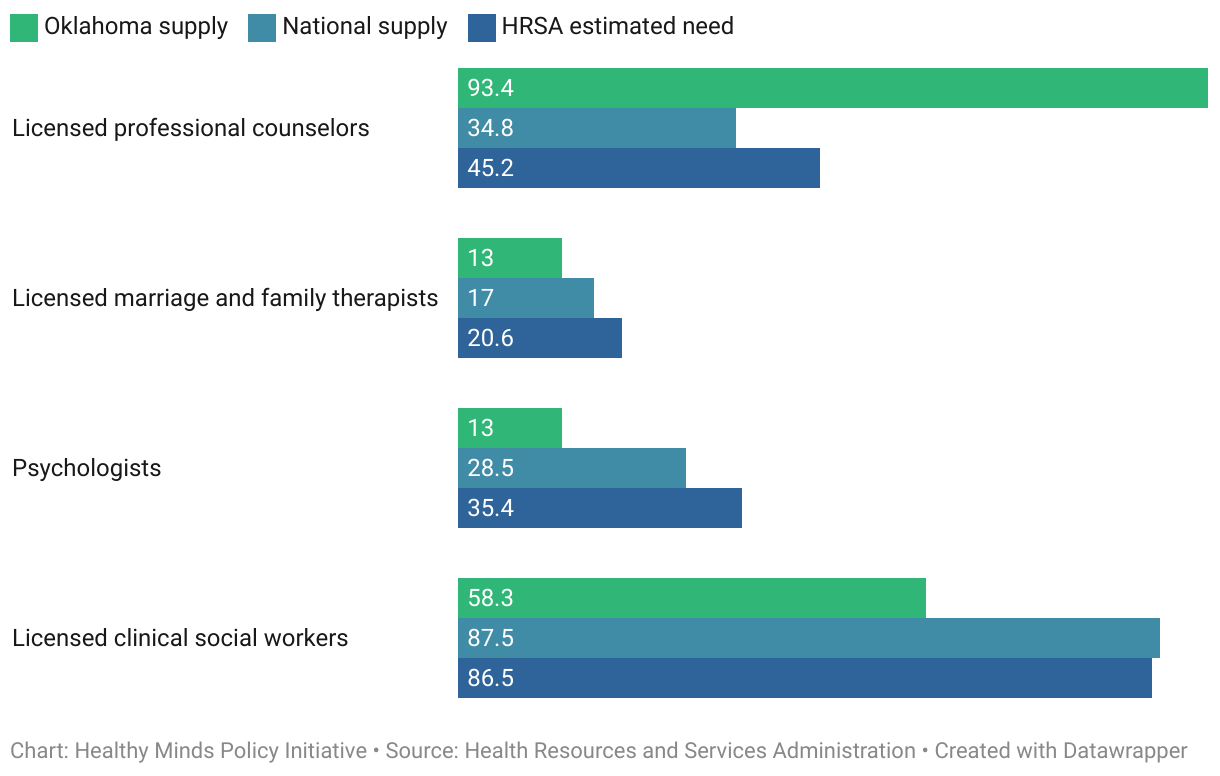
Except for licensed professional counselors (LPCs), all psychosocial behavioral health providers are also in short supply in Oklahoma.
According to state licensure data, the number of LPCs in Oklahoma exceeds the national supply estimate and is double HRSA’s estimated need. We cannot know how many LPCs are working in the field, and if they are, whether they are working full- or part-time. However, LPC licensure data does include geographic distribution, which shows an adequate supply in all regions (northwest, northeast, southwest, and southeast) and both Tulsa and Oklahoma counties. All regions surpass both HRSA’s estimated need and the national supply, though some to a much greater extent than others.
Strengthening Oklahoma’s pipeline of behavioral health professionals
Read the full report
Degree programs supporting behavioral health careers are graduating more students than ever, but not enough to meet the state’s growing need for treatment services after workforce attrition. These programs also do not meet current demand for these careers among prospective students, and regularly turn down competitive applicants due to space and funding limitations.
In-state training opportunities are particularly limited for the most-needed, most highly trained behavioral health professions — psychiatry and psychology. A limited number of residency training positions for psychiatrists prevents most medical school graduates from completing training in their chosen discipline of psychiatry in the state. Oklahoma would need to more than double its number of psychiatric residency slots to match the current national average of psychiatrists within 10 years. Opportunities for psychologists-in-training to complete their pre-doctoral internships in Oklahoma are limited, forcing many graduates to complete their training out of state. This decreases the likelihood that they will return to work in Oklahoma.
Potentially hindering recruitment and quality, 75% of Oklahoma master’s programs for licensed professional counselors, licensed marriage and family therapists, and licensed alcohol and drug counselors are unaccredited. Attending an unaccredited program can cause challenges for students in obtaining licensure and employment. Because unaccredited programs are not held to rigorous standards, they may under-prepare students to serve clients. Unaccredited programs are also less likely to attract out-of-state students than accredited programs.
Paraprofessionals such as peer recovery support specialists, psychiatric technicians, and behavioral health case managers are an untapped resource. Actively encouraging these individuals to pursue professional degrees would reduce the gap between the supply of and demand for psychosocial behavioral health professionals.