Proposed federal parity rules would strengthen access to care for Oklahomans
Despite more mental health need than ever in the U.S., people seeking treatment for mental illness or addiction still face barriers to accessing lifesaving care.
One common hurdle is how health plans impose limits on mental health or substance use treatment that don’t apply to physical health care services, indicating a lack of parity in how insurers cover mental and physical health care.
This lack of parity is evident when people seeking mental health and addiction treatment are forced to go out of network for the care they need: research has shown this happens at least seven times more often for behavioral health office visits than for similar physical health care appointments.
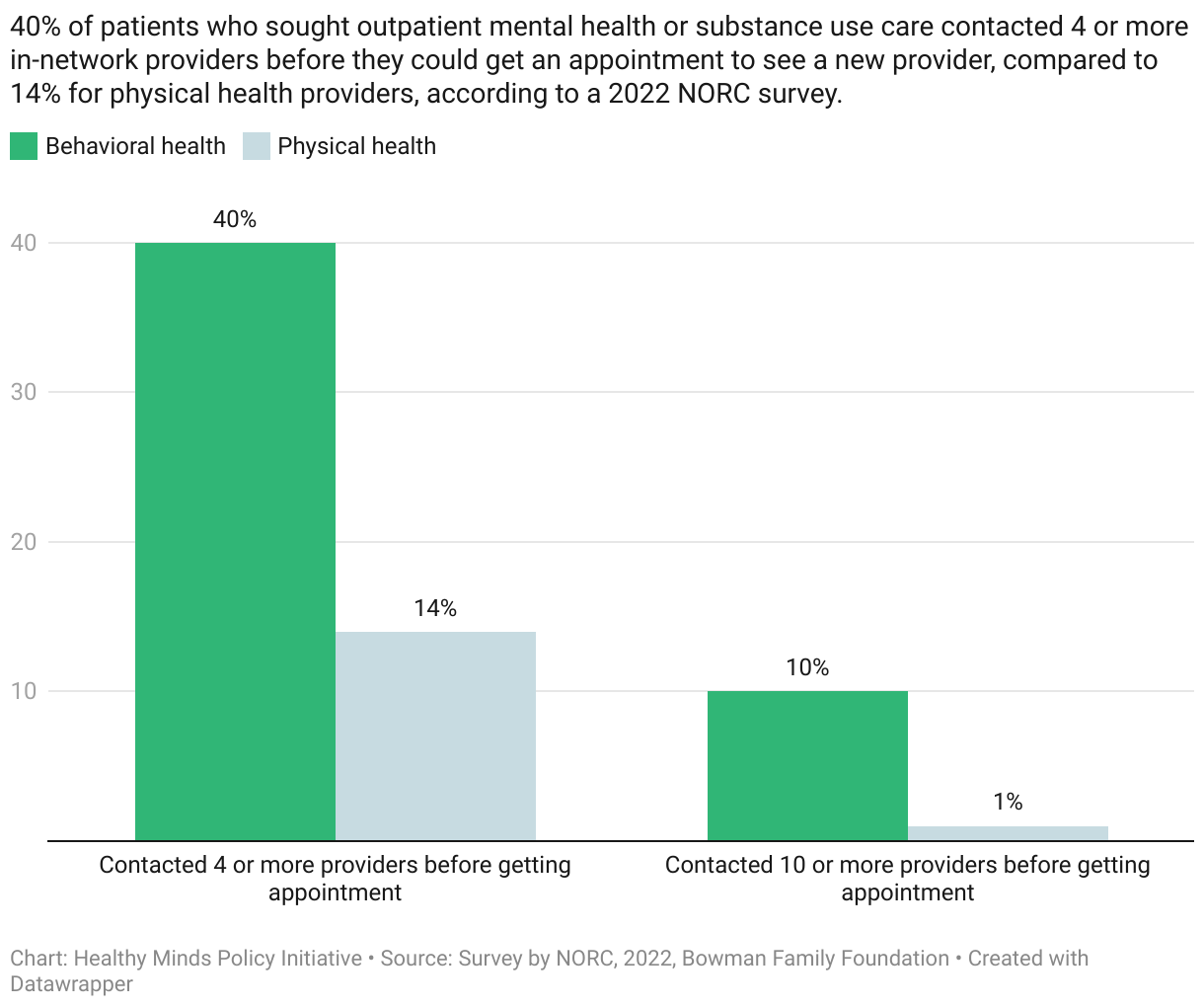
Inadequate provider networks for behavioral health care can also force patients to contact many providers before getting an appointment, a process that can be frustrating and time-consuming. A 2022 survey by NORC, commissioned by The Bowman Family Foundation, found a stark disparity in how many patients seeking outpatient behavioral health care had to contact four or more providers to get an appointment, compared to patients seeking a physical health provider.
Providers contacted before getting appointment with new provider, physical vs. behavioral health
The report also cited recent Healthy Minds research examining access to behavioral health care through commercial insurance in Oklahoma, which found significant shortcomings and barriers for patients.
Though current mental health parity laws require equitable insurance coverage for mental and physical health care, unclear regulations have left federal and state entities struggling to implement and enforce them. But new proposed rules from the U.S. departments of Labor, the Treasury, and Health and Human Services would strengthen the enforcement of a federal parity law, the Mental Health Parity and Addiction Equity Act, or MHPAEA, which would mean better access to care in Oklahoma and beyond.
What the rule changes would do
The proposed rules would require insurers to analyze their approval and denial rates of mental health services and compare them to rates for medical and surgical services. If the analysis showed that insurers denied more behavioral health services than they did medical and surgical services, a regulator could hold the insurance carrier accountable for violating mental health parity laws.
The rules would also require insurance carriers to review their provider networks and compare their reimbursement rates for mental health versus medical and surgical benefits for out-of-network providers. On top of shortages of mental health providers, many existing mental health providers don’t participate in insurance networks. Insurers have an opportunity to incentivize providers’ participation in insurance networks, which in turn will help people seeking treatment get the care they need.
The proposed rules also address prohibited prior authorization and other medical management techniques often used by insurers to cut costs, sometimes at the detriment of people seeking timely care.
Taken as a whole, the proposed rules aim to strengthen provider networks and lessen restrictions that keep people from accessing mental health and addiction care they need.
Though these are proposed changes to federal rules, they would also impact parity in Oklahoma. State law requires insurance plans to comply with any additional federal guidance or regulation under MHAPEA, and the increased clarity in the proposed rules would help Oklahoma insurers more easily comply with parity requirements.
Federal and state parity laws affecting Oklahoma
Congress passed the nation’s first parity law, the Mental Health Parity Act, in 1996, and Oklahoma followed suit with a state law in 1999. These initial laws had significant loopholes and did not require health plans to cover mental health treatment.
In 2008, Congress passed the Mental Health Parity and Addiction Equity Act (MHPAEA), which required all large-group employer-sponsored insurance plans to cover mental health services at parity with medical or surgical services if they offered mental health coverage at all. The law also closed the Mental Health Parity Act’s loopholes and expanded parity to substance use treatment. Soon after, in 2009, the Affordable Care Act mandated coverage for mental health and substance use treatment for individual and small-group insurance plans.
In Oklahoma, Gov. Kevin Stitt signed the state’s first mental health parity reporting bill in 2020. Senate Bill 1718 requires the Oklahoma Insurance Department to monitor health plans’ compliance with federal law. There are currently no enforcement mechanisms in state statute, leaving federal agencies responsible for ensuring insurance plans follow the law.
After Oklahoma passed its 2020 parity law, federal agencies changed their reporting guidelines. To better align with federal law and reduce reporting burdens on health plans, Gov. Stitt signed Senate Bill 1413 in 2022, which also says insurance companies must comply with any new federal regulations under MHPAEA in the future.
What’s next
The proposed changes are not final. Currently, the rules are open for public comment until Oct. 2.
Federal agencies that proposed the rules will then review the comments, including those from insurers and mental health advocates, and have a chance to make any changes they deem necessary. From there, the Federal Register would publish a final rule, and soon after that, the rules would take effect.
Establishing parity between mental and physical health care is not only crucial to the prevention and treatment of behavioral health disorders – it's the law. The proposed federal rules bring the nation, and Oklahoma, one step closer to ensuring people have the mental health treatment they need, when and where they need it.