National parity study finds persistent, pervasive barriers to mental health care in Oklahoma, U.S.
A new report examining parity between mental and physical health care services on commercial insurance plans found persistent, pervasive disparities in Oklahoma and across the U.S. that force people out-of-network to access behavioral health care and underpay mental health providers compared to their physical health counterparts.
The study, conducted by the Research Triangle Institute (RTI) International and commissioned by The Bowman Family Foundation, used health insurance claims data from 2019 through 2021 for comparisons at the state and national levels.
The report found that Oklahomans must go out-of-network for behavioral health care far more often than they do for physical health care — 55% more often for office visits, where most behavioral health care is provided, and even greater disparities exist at higher levels of care. The study also found disparities in how insurance plans pay behavioral health providers compared to physical health providers. In Oklahoma, behavioral health clinicians are reimbursed 22% less for office visits than for similar physical health visits.
Federal and Oklahoma law requires mental health and substance use disorders be treated just like any other health condition — insurance providers must offer equal insurance coverage of both mental and physical health services.
But poor and inconsistent compliance and enforcement of these laws leave patients to grapple with inadequate networks of behavioral health providers, long waits for care, and higher costs when they’re forced to see an out-of-network provider.
"The data continue to validate the experiences of countless Americans who have struggled to find mental health providers through their commercial health plans,” said Zack Stoycoff, executive director at Healthy Minds Policy Initiative. “The disparities highlighted by RTI International and The Bowman Family Foundation are some of the most important barriers to mental health services across the country, demanding strong action by policymakers, employers, and health plans."
The RTI International study found much higher use of out-of-network providers for behavioral health services compared to medical-surgical (or physical) health services.
Out-of-network utilization for behavioral health vs. physical health office visits
The report’s finding that Oklahomans went out-of-network 1.4 times more for outpatient behavioral health visits than for similar physical health visits in 2021 was an improvement from an earlier report by the risk management firm Milliman. While the two studies were not identical, 2017 data from the Milliman report found that Oklahomans went out-of-network 9 times more for such visits.
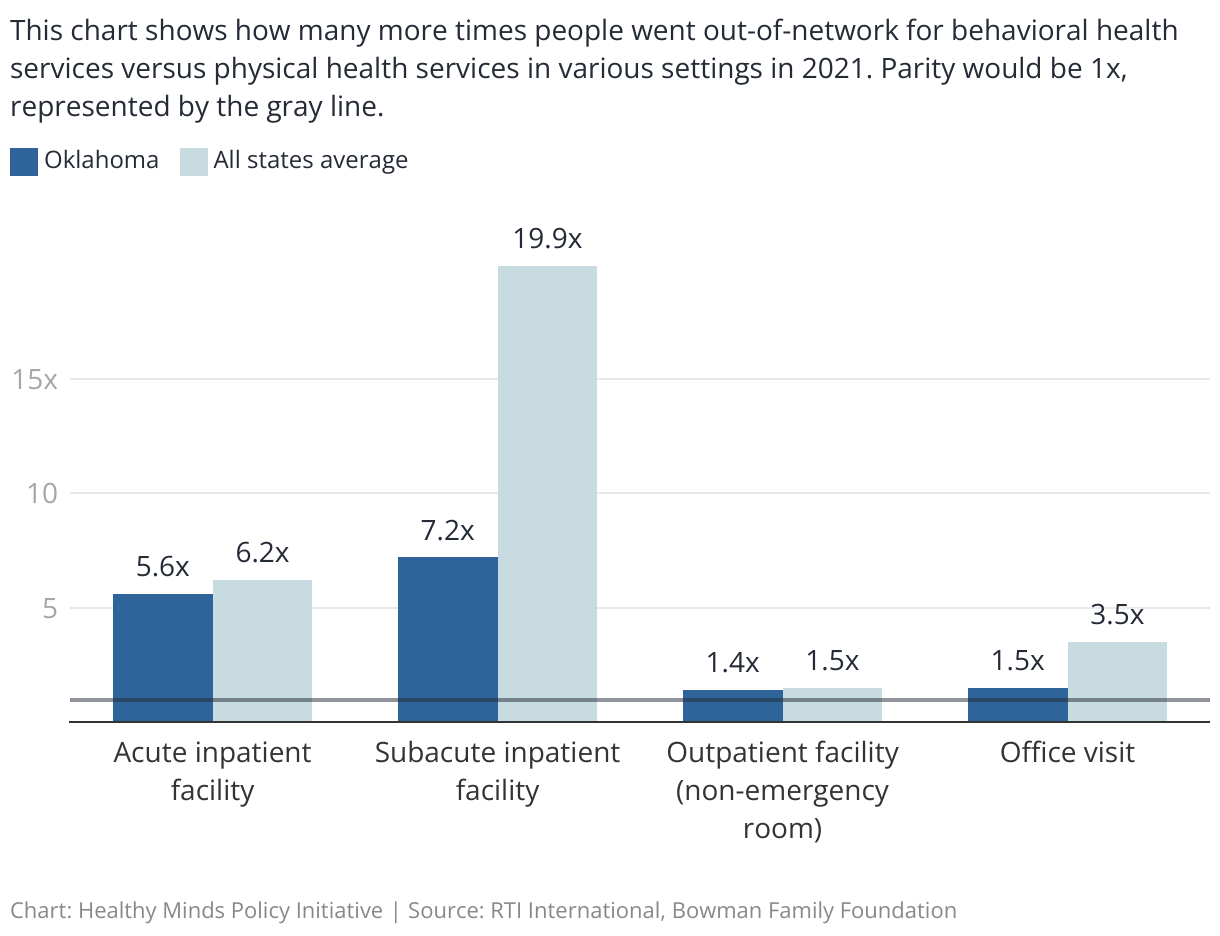
Despite some improvements, the report showed significant barriers to accessing behavioral health care in Oklahoma. These disparities are even more pronounced at higher levels of care: in 2021, Oklahomans went out-of-network over 5 times more often for behavioral health care in acute inpatient settings and over 7 times more for subacute inpatient settings.
Oklahoma and U.S. out-of-network utilization for behavioral health vs. physical health services
Nationally, people went out-of-network for an office visit with a behavioral health clinician 3.5 times more in 2021 than they did for a physical health office visit. In 2013 data from the Milliman report, behavioral health office visits were 3.7 times more likely to be out-of-network than physical health ones, showing only a slight improvement in the past nine years.
The report recommends that insurance companies shore up their provider networks, incentivizing behavioral health providers to join networks by offering higher reimbursement rates.
Healthy Minds’ 2023 network adequacy study found that lower reimbursement rates disincentivized providers from participating in commercial insurance networks, contributing to Oklahoma’s inadequate networks of behavioral health providers. In the best health plan example studied, only 30% of behavioral health professionals were in-network.
Since its inception, Healthy Minds has championed laws that improve Oklahomans’ access to mental health care through parity.
In 2023, Healthy Minds worked with lawmakers to pass Senate Bills 442 and 254, which address high patient costs and excessive wait times for appointments by ensuring more transparency from commercial health insurance plans and capping out-of-pocket costs when a timely appointment with an in-network provider isn’t available.
Healthy Minds also advocated for the passage of Senate Bill 1413 in 2022, which aligned state parity reporting requirements with federal requirements, strengthening the state’s ability to enforce parity in insurance coverage.
Oklahoma can continue its leadership on state-level parity reform by addressing provider reimbursement rates, as the report recommends. In doing so, the state can ensure more Oklahomans can access the mental health and substance use treatment they need.